Treatment options
Treatment options
At The Focal Therapy Clinic, we provide both focal therapy treatments for prostate cancer — high-precision, revolutionary treatments based upon advanced diagnostics for men with early to intermediate stage prostate cancer which is confined to the prostate gland:
- HIFU, or high-intensity focused ultrasound – an extremely safe and effective focal therapy for medium and large-volume cancers in the lower prostate. Cancer cells are targeted with unrivalled accuracy and surrounding healthy tissues are unaffected, with little to no side effects
- NanoKnife, or Irreversible Electroporation (IRE) – high-precision focal therapy used to treat early to intermediate-stage cancer in areas of the prostate that are hard to reach using HIFU. Patients experience few side effects, if any
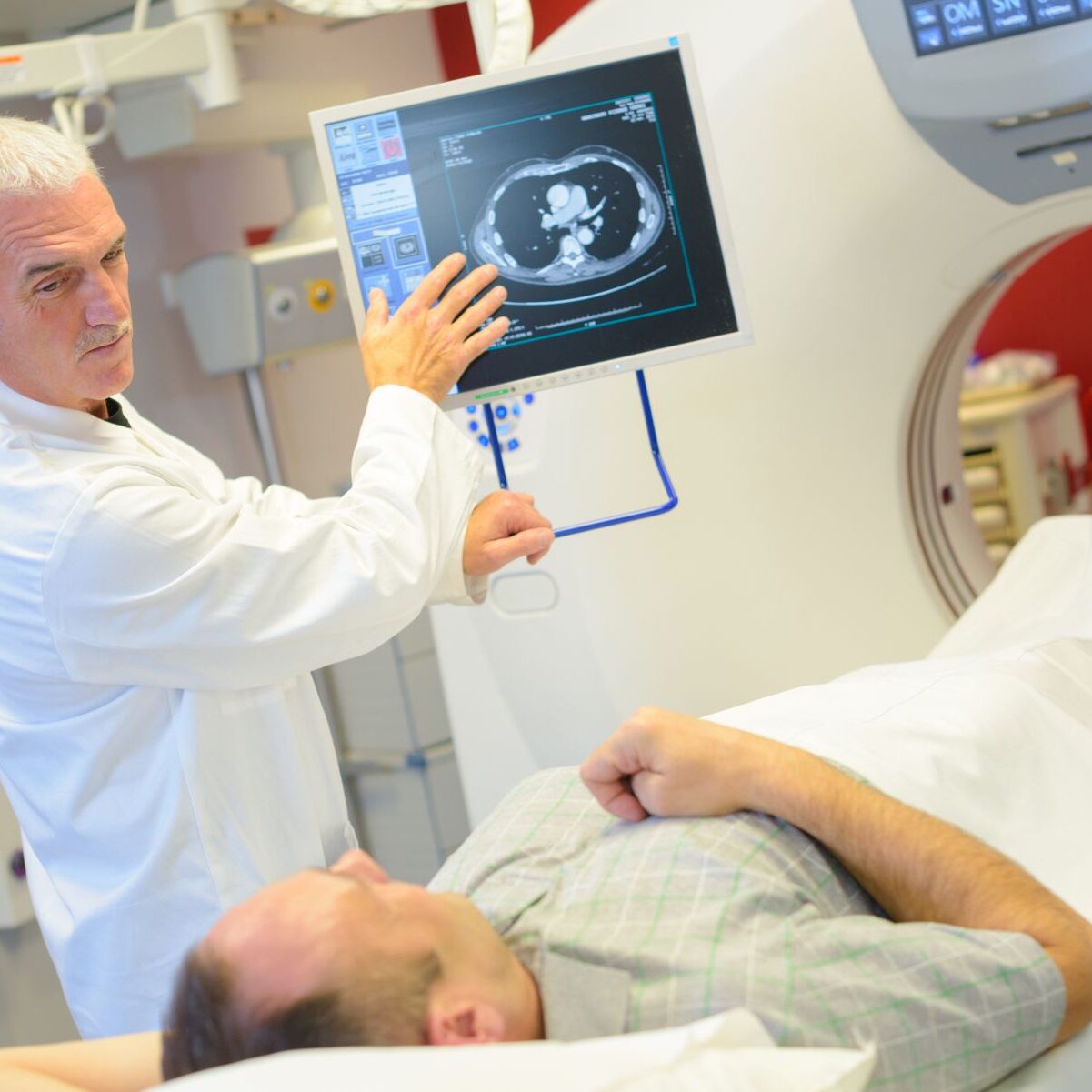



We believe that all men should have the greatest possible choice over their prostate cancer treatment. The right treatment for you will depend on your circumstances. Some patients may not need any treatment, while for others, treatment will help to control or cure the disease. Our goal is to ensure that patients maintain optimal quality of life despite their prostate cancer.
Traditional prostate cancer treatments include:
- Active surveillance – watching and waiting to see if the cancer grows to a stage where treatment is required.
- Radiotherapy – a common treatment often recommended for localised prostate cancer that uses radiation to destroy cancer cells
- Hormone therapy – often used in combination with radiotherapy, hormone therapy is used to slow the progression of advanced prostate cancers and relieve symptoms
- Chemotherapy – usually only recommended when prostate cancer has spread to other parts of the body
- Radical prostatectomy – surgical removal of the prostate gland, recommended for localised cancer; the main side effect is your ability to have children
“Active surveillance may be highly effective in monitoring cancer, but for me, it was doing my head in — constantly worrying, not sleeping properly, and with my mind taking me to some very dark places.”
Perry Letcher, The Focal Therapy Clinic patient
 Statistics
Statistics
52,000
Diagnosed in the UK every
year. 143 men daily
47,000 +
Diagnosed annually
in England
12,039
51%
16%
 Additional resources
Additional resources
Want to know more?
Our team are here to answer any questions.
Any questions?
Being diagnosed with prostate cancer can be very distressing, and it’s normal to feel anxious, fearful and unsure which treatment to choose. We understand the emotions you may be experiencing and are here to help you to make a confident, informed decision about your care.
If you've got any questions about your prostate cancer diagnosis or want to know more about HIFU or NanoKnife focal don’t hesitate to get in touch with our friendly, knowledgeable team.
Fill in an enquiry form

