Prostate cancer resources
What is prostate cancer?
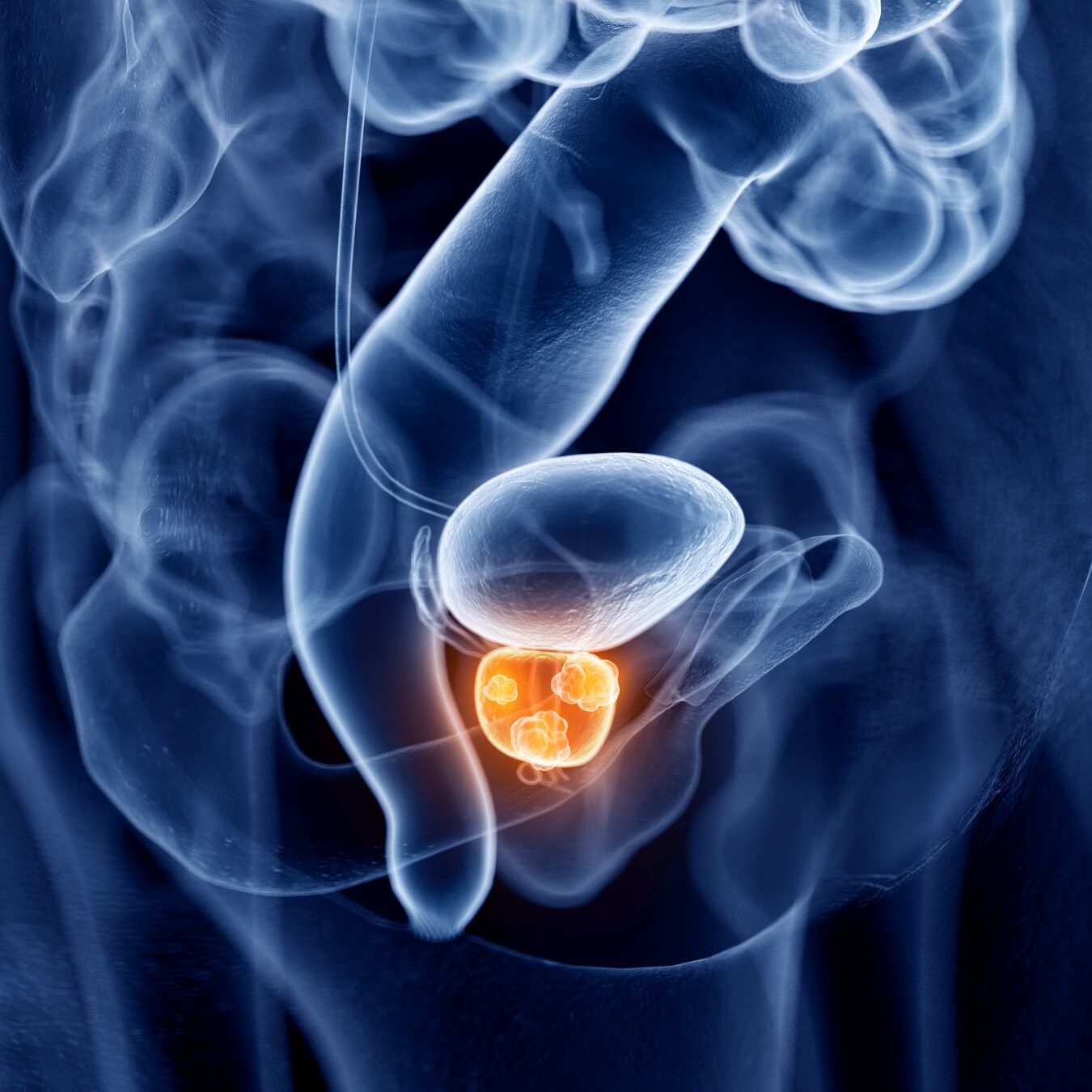
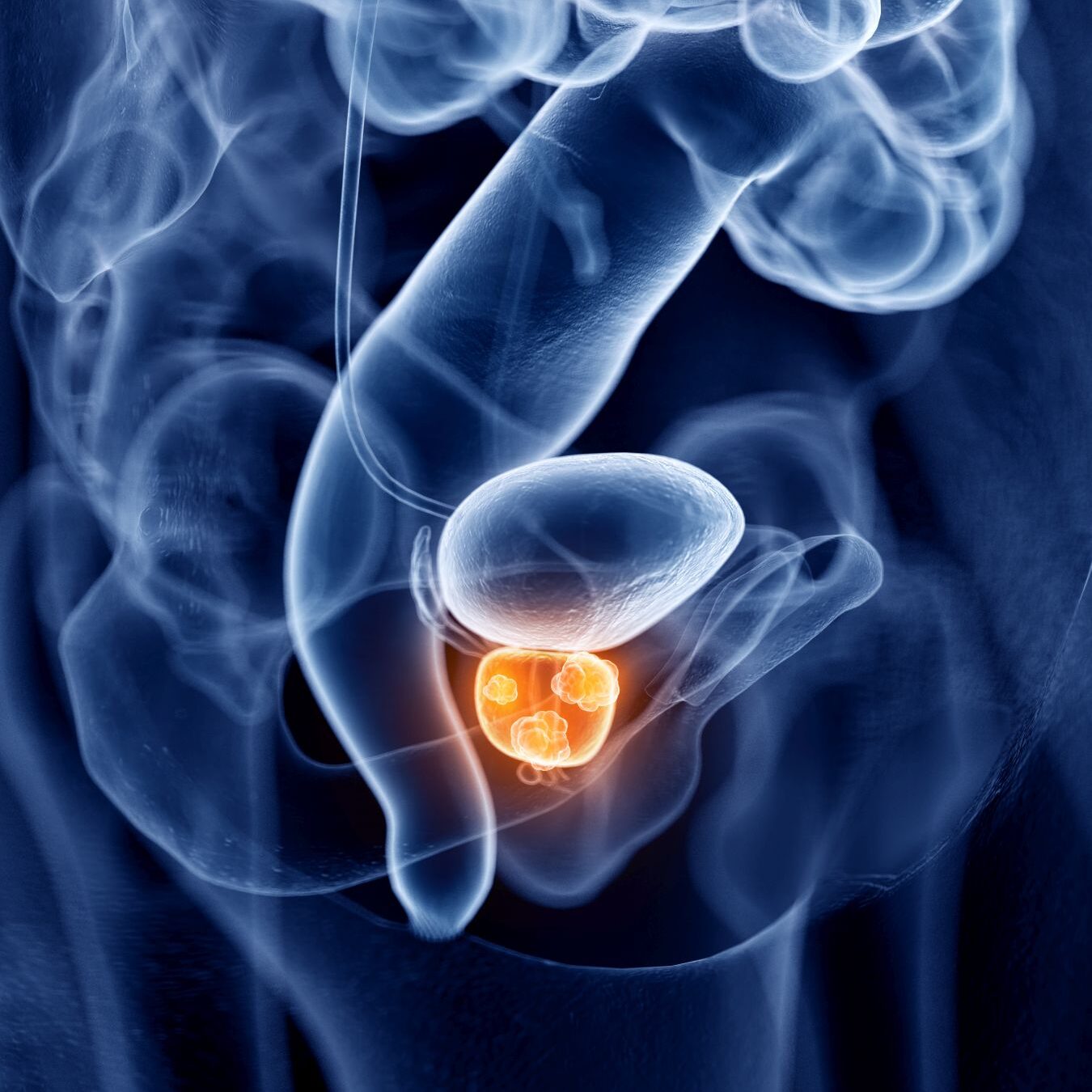
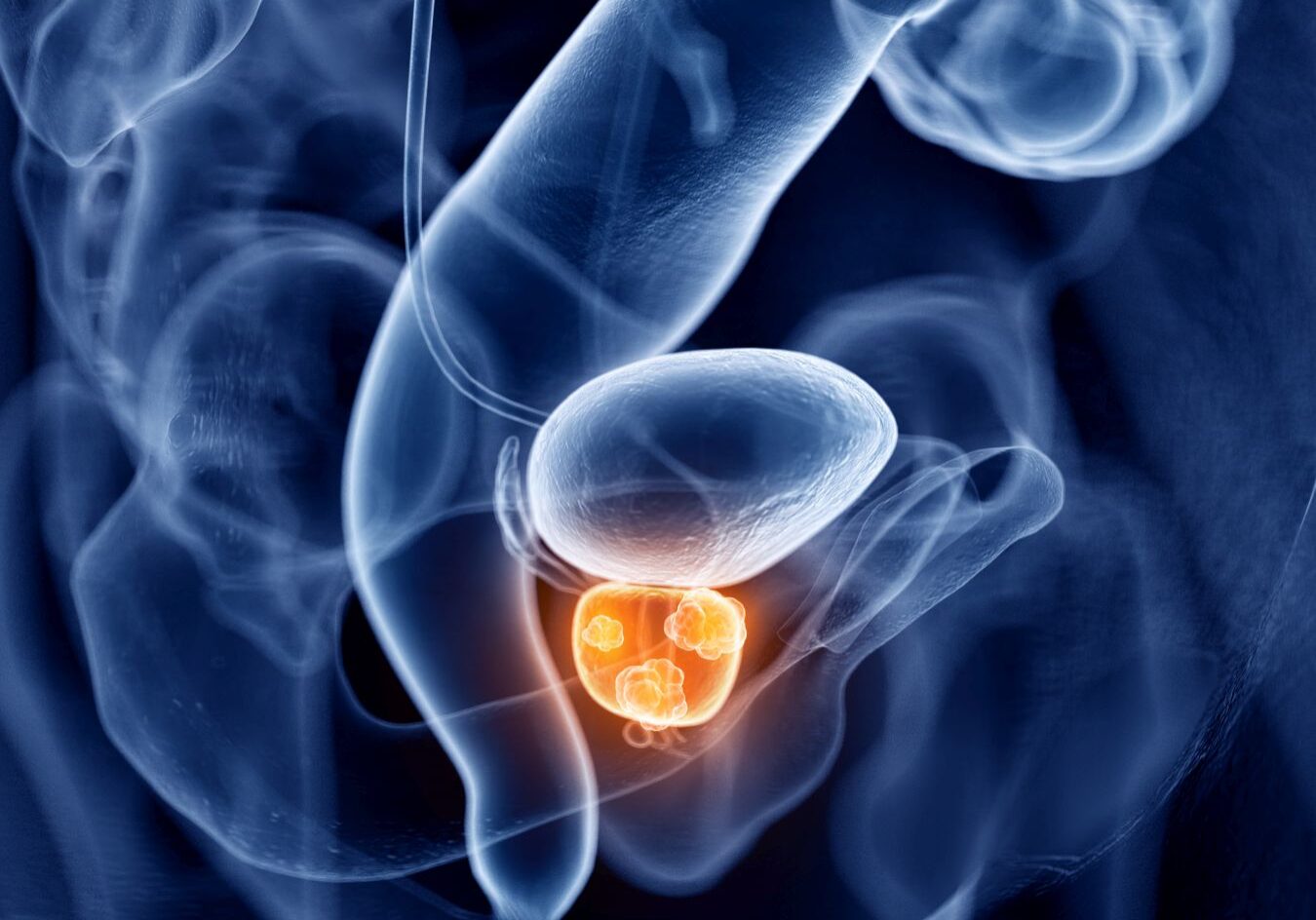
Prostate cancer is a cancer that occurs in a part of the male body called the prostate, which is located just below your bladder and in front of your rectum. It is about the size of a walnut and surrounds the urethra — the tube that carries urine out of your body. The role of the prostate is to produce fluid that will form part of semen.
Prostate cancer occurs when some of the cells within the prostate become abnormal and start to divide and grow in an uncontrolled way. Initially, this will be localised to the prostate, but the cells can eventually grow into surrounding tissues and organs, before spreading to other parts of the body.
Prostate cancer is the most common cancer in men in the UK with about 1 in 8 men being diagnosed with the disease in their lifetime.
 Statistics
Statistics
52,000
Diagnosed in the UK every
year. 143 men daily
47,000 +
Diagnosed annually
in England
12,039
pre-mature deaths
from prostate cancer
51%
51% with early to intermediate prostate cancer at diagnosis
16%
16% with metastatic disease at initial diagnosis
 Additional resources
Additional resources
Tim Dudderidge discussing how Focal Therapy had emerged as a middle ground treatment for Prostate Cancer.
(1:50)
Want to know more?
Our team are here to answer any questions.
Any questions?
Being diagnosed with prostate cancer can be very distressing, and it’s normal to feel anxious, fearful and unsure which treatment to choose. We understand the emotions you may be experiencing and are here to help you to make a confident, informed decision about your care.
If you've got any questions about your prostate cancer diagnosis or want to know more about HIFU or NanoKnife focal don’t hesitate to get in touch with our friendly, knowledgeable team.
Fill in an enquiry form

